Achieving High Convection Volumes in Online Hemodiafiltration (OL-HDF)
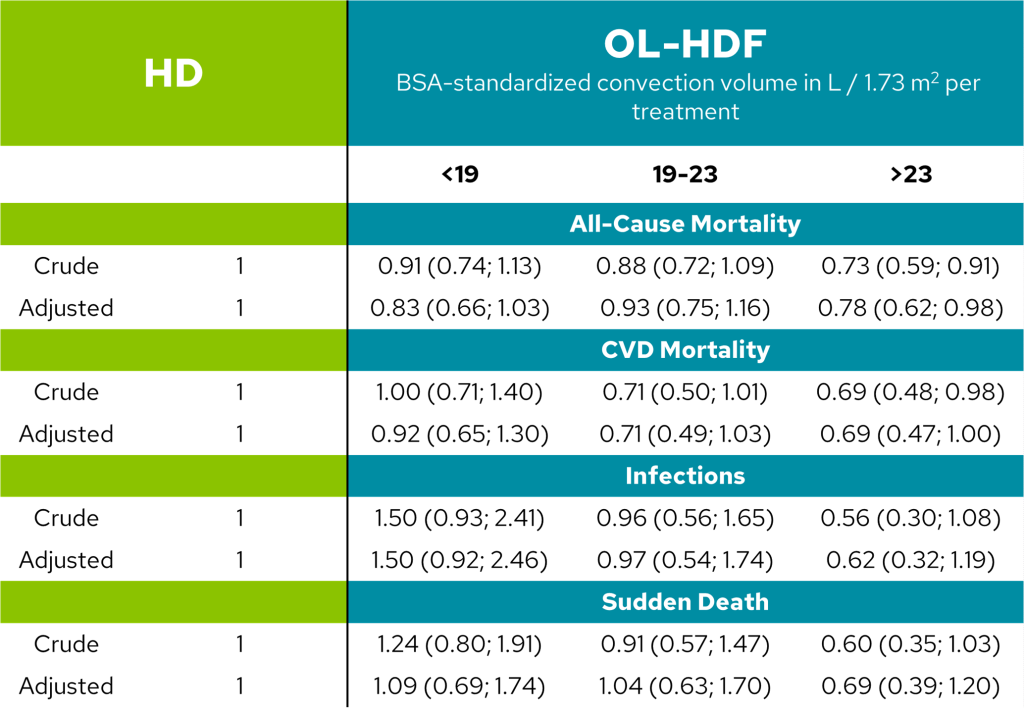
Several randomized controlled trials and a pooled individual participant data analysis of four of these trials have shown that convection volumes ≥23 L per session per 1.73 m2 body surface area (≥21 L substitution volume + 2 L net ultrafiltration) is associated with improved clinical outcomes compared to conventional hemodialysis (Table 1) (1)–(6).
Table 1. All-cause mortality decrease in tertile receiving highest, BSA-standardised convection volume (5) (p.981).
A number of factors can affect the level of convection volume achieved. These include both patient characteristics, such as vascular access type, vascular access flow, total protein level, and hematocrit, and modifiable factors associated with the dialysis prescription and best nursing care practices, such as the dialyzer type, the selected arterial and venous needles, level of blood flow rate (within the limit allowed by the vascular access), and the duration of the dialysis session.
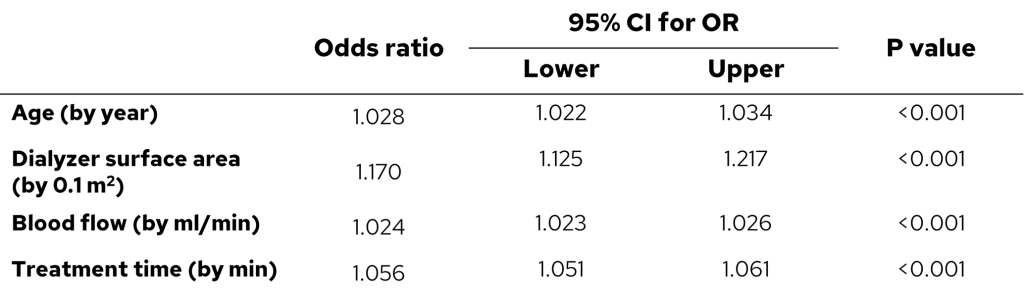
For example, Marcelli D et al., investigated factors associated with the successful achievement of ≥21 l/session of substitution fluid volume in 3,315 patients treated in 6 European countries on post-dilution hemodiafiltration (Table 2) (7). The authors reported that the mean blood flow rate was 379 ± 68 ml/min and the median substitution volume was 24.7 L. The mean filtration fraction was 28.3 ± 4.1% and 81.5% of sessions qualified as high-volume HDF (substitution volumes ≥21 L). In this study, higher age, dialyzer surface area, blood flow rate, and treatment time were positively associated with the achievement of ≥21 L substitution volume whereas higher body mass index, male gender, higher hematocrit, graft or catheter versus fistula, and start of week versus mid-week were negatively associated.
Table 2. Factors associated with achievement of ≥21 L/session substitution volume (7) (p.247).
Additionally, Chapdelaine I et al., demonstrated that treatment time and blood flow rate were major determinants of convection volume (8). Penne EL et al., evaluated potential patient- and treatment-related determinants of convective volume in 235 patients on post-dilution HDF using multivariable linear regression models (9). The authors concluded that, in addition to treatment time and blood flow rate, convective volumes may be optimized by increasing filtration fraction.
Several studies have demonstrated that stepwise adjustment of the factors that affect convection volume can be used to achieve convection volume targets associated with improved outcomes (10,11). One such study prospectively investigated the feasibility of achieving and maintaining high convection volumes with online post dilution HDF (high-volume HDF, defined as ≥22 L convection volume/session) in everyday clinical practice, irrespective of preexisting patient profiles (10). In a stepwise fashion, treatment time, blood flow rate and filtration fraction were optimized. After the optimization phase, 71/86 participants (83%) reached a convection volume of ≥22 L/session (mean 25.5 ± 3.6). In the maintenance phase, at week 4, 64/86 participants (74%) reached a convection volume of ≥22 L/session compared to 66/83 (80%) at week 8. Mean convection volumes at week 4 and 8 were 26.2 ± 3.6 and 26.0 ± 3.4 L/session, respectively (Figure 1).
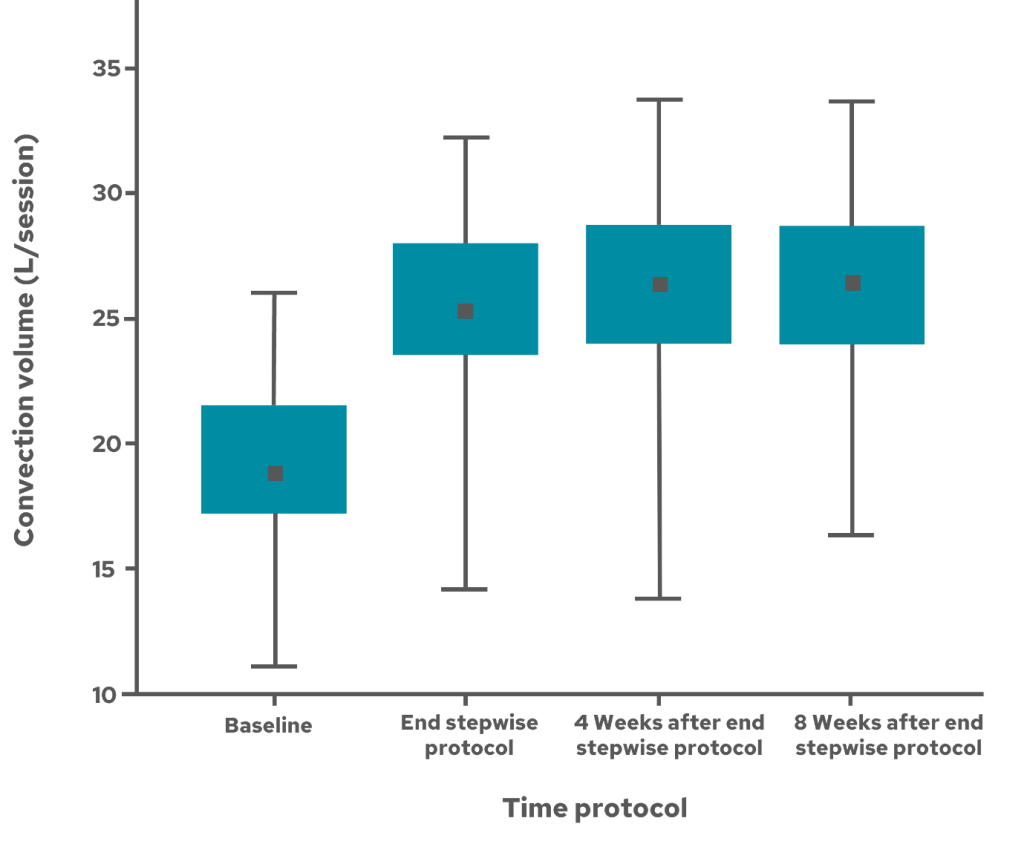
Figure 1. Stepwise optimisation of treatment time, blood flow rate, and filtration fraction in achieving high-volume OL-HDF (10) (p.809).
In this study 79% of 4,176 sessions were classified as high-volume HDF (≥21 L substitution volume/session, corresponding to 23.4 L convection volume/session). The patients achieved high convection volume irrespective of age, body size or comorbidities. Only, incremental adjustments in blood flow rate and filtration fraction alone were sufficient to obtain the high convection volume (10). Importantly, the high convection volumes were not associated with undesirable pressure changes. However, the study is limited due to selection bias and the blood flow was not independently checked.
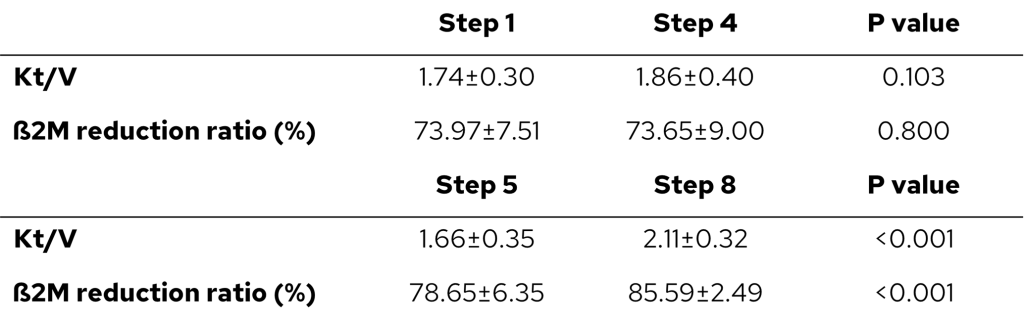
Another prospective study aimed to optimize methods for achieving a high convection volume in patients undergoing online HDF (11). This study investigated 30 patients undergoing hemodialysis, where a stepwise protocol was implemented by gradually increasing the blood flow rate (280 to 300 to 330 ml/min; steps 1, 2, and 3) and needle size (16 to 15 G; step 4). After changing dialyzer surface area (1.8 m2 to 2.5 m2), the blood flow rate and needle size were similarly increased stepwise (steps 5, 6, 7, and 8). The mean substitution volume was 18.7 ± 2.2 L at step 1 and it significantly increased to 25.1 ± 2.6 L by step 8. A substitution volume of 21 L was achieved by 13.3% of patients in step 1 and by 96.7% after step 8. The substitution volume was higher for the dialyzer with a large surface area and for the larger needle (15 G). Between steps 1 and 8, the Kt/V and β2microglobulin reduction ratios also improved significantly.
Table 3. Increase of Kt/V and ß2M RR in higher convection volumes (11) (p.371).

The study demonstrated that an increase in the convection volume can be obtained independent of the patient’s clinical characteristics, through a structured, stepwise protocol with an incremental adjustment of blood flow rate, needle size and using a dialyzer with a large surface area (11). However, the study is limited due to small sample size and using only two kinds of dialyzer and needle size, hence it does not represent the clinical practice in real world.
In summary, the convection volumes that are achieved during OL-HDF are affected by both patient characteristics (e.g., vascular access type, vascular access flow, total protein level, and hematocrit) and modifiable factors (e.g., the dialyzer type, the selected arterial and venous needles, level of blood flow rate [within the limit allowed by the vascular access], and the duration of the dialysis session). Stepwise adjustment of the modifiable factors can help to achieve the convection volume targets associated with improved outcomes.
References:
- Ok E, Asci G, Toz H, Ok ES, Kircelli F, Yilmaz M, Hur E, Demirci MS, Demirci C, Duman S, Basci A, Adam SM, Isik IO, Zengin M, Suleymanlar G, Yilmaz ME, Ozkahya M. Mortality and cardiovascular events in online haemodiafiltration (OL-HDF) compared with high-flux dialysis: results from the Turkish OL-HDF Study. Nephrol Dial Transplant. 2013;28(1):192-202. www.ncbi.nlm.nih.gov/pubmed/23229932
- Grooteman MPC, van den Dorpel MA, Bots ML, Penne EL, van der Weerd NC, Mazairac AHA, den Hoedt CH, van der Tweel I, Lévesque R, Nubé MJ, ter Wee PM, Blankestijn PJ. Effect of online hemodiafiltration on all-cause mortality and cardiovascular outcomes. J Am Soc Nephrol. 2012;23(6):1087-96. www.ncbi.nlm.nih.gov/pubmed/22539829
- Maduell F, Moreso F, Pons M, Ramos R, Mora-macià J, Carreras J, Soler J, Torres F, Campistol JM. High-Efficiency Postdilution Online Hemodiafiltration Reduces All-Cause Mortality in Hemodialysis Patients. JASN. 2013:487-497.
- Morena M, Jaussent A, Chalabi L, Leray-Moragues H, Chenine L, Debure A, Thibaudin D, Azzouz L, Patrier L, Maurice F, Nicoud P, Durand C, Seigneuric B, Dupuy A-M, Picot M-C, Cristol J-P, Canaud B, FRENCHIE Study Investigators A, Aguilera D, et al. Treatment tolerance and patient-reported outcomes favor online hemodiafiltration compared to high-flux hemodialysis in the elderly. Kidney Int. 2017;91(6):1495-1509. www.ncbi.nlm.nih.gov/pubmed/28318624
- Peters SAE, Bots ML, Canaud B, Davenport A, Grooteman MPC, Kircelli F, Locatelli F, Maduell F, Morena M, Nubé MJ, Ok E, Torres F, Woodward M, Blankestijn PJ, HDF Pooling Project Investigators. Haemodiafiltration and mortality in end-stage kidney disease patients: a pooled individual participant data analysis from four randomized controlled trials. Nephrol Dial Transplant. 2016;31(6):978-84. www.ncbi.nlm.nih.gov/pubmed/26492924
- Blankestijn PJ, Vernooij RWM, Hockham C, Strippoli GFM, Canaud B, Hegbrant J, Barth C, Covic A, Cromm K, Cucui A, Davenport A, Rose M, Török M, Woodward M, Bots ML. Effect of Hemodiafiltration or Hemodialysis on Mortality in Kidney Failure. N Engl J Med. 2023. GMO-000780 Rev A 09-8-2023. www.ncbi.nlm.nih.gov/pubmed/37326323
- Marcelli D, Kopperschmidt P, Bayh I, Jirka T, Merello JI, Ponce P, Ladanyi E, Benedetto A Di, DovcDimec R, Rosenberger J, Stuard S, Scholz C, Grassmann A, Canaud B. Modifiable factors associated with achievement of high-volume post-dilution hemodiafiltration: Results from an international study. Int J Artif Organs. 2015;38(5):244-250. www.ncbi.nlm.nih.gov/pubmed/26080930
- Chapdelaine I, Mostovaya IM, Blankestijn PJ, Bots ML, van den Dorpel MA, Lévesque R, Nubé MJ, ter Wee PM, Grooteman MPC, CONTRAST investigators. Treatment Policy rather than Patient Characteristics Determines Convection Volume in Online Post-Dilution Hemodiafiltration. Blood Purif. 2014;37(3):229-237. www.ncbi.nlm.nih.gov/pubmed/24943743
- Penne EL, van der Weerd NC, Bots ML, van den Dorpel MA, Grooteman MPC, Levesque R, Nube MJ, ter Wee PM, Blankestijn PJ, CONTRAST investigators. Patient- and treatment-related determinants of convective volume in post-dilution haemodiafiltration in clinical practice.Nephrol Dial Transplant. 2009;24(11):3493-3499. www.ncbi.nlm.nih.gov/pubmed/19515802
- De Roij van Zuijdewijn CLM, Chapdelaine I, Nubé MJ, Blankestijn PJ, Bots ML, Konings CJAM, Hovinga TKK, Molenaar FM, van der Weerd NC, Grooteman MPC. Achieving high convection volumes in postdilution online hemodiafiltration: A prospective multicenter study. Clin Kidney J. 2017;10(6):804-812.
- Kim DH, Lee Y-K, Park HC, Kim J, Yun KS, Cho Aj, Noh J-W, Kim H, Kim S-H, Yoon J-W. Stepwise achievement of high convection volume in post-dilution hemodiafiltration: A prospective observational study. Semin Dial. 2021;00:1-7. www.ncbi.nlm.nih.gov/pubmed/33774852
GMO-000780 Rev A 06/2024
