History of HHD and Current Trends
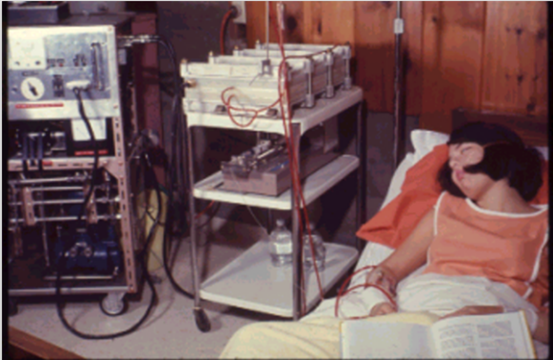
Figure 1. One of the first Home HD patients. Photo courtesy of Dr. Blagg.
A Brief History
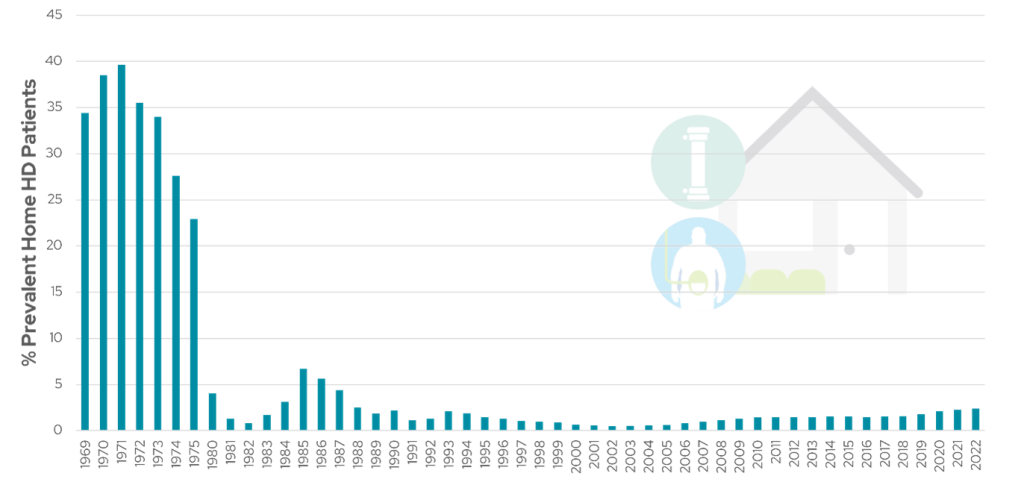
Interest in home hemodialysis (HHD) began during the early 1960s, not long after Dr. Belding Scribner developed the Scribner shunt and enabled hemodialysis as a long-term treatment modality for chronic kidney disease (CKD) patients. In the early days of HD, dialyzing at home was a popular choice for many patients, who experienced improved rehabilitation at less than half the cost of those dialyzing in-center1. Figure 1 shows a photo of one of the first HHD patients dialyzing at home, who did not meet criteria for in-center hemodialysis (ICHD). At its peak in the early 1970s, HHD was used by 40% of patients in the United States (Figure 2)1.
The enactment of the Medicare End Stage Renal Disease (ESRD) Program by Congress in 1972 marked the first time Medicare patients under 65 with Stage 5 CKD could receive Medicare benefits. This led to more patients with access to chronic dialysis treatment and stimulated the rapid expansion of ICHD facilities, where previously these had been a scarce resource. ICHD rapidly became the preferred modality, while the number of patients utilizing HHD plummeted, reaching 1.3% in 19812 and even further to 0.48% in 2002 (Figure 2)3.
Figure 2: Percentage of prevalent US dialysis patients on home hemodialysis from 1969-2022 (Adapted from Bryan et al2, and USRDS 2024 ADR3).
Similarly to the US, most European countries around the same time favored in-center-based care, both for the profitability of in-patient dialysis as well as the potential for liability for patients performing complex treatments without physician supervision4. By contrast, at the same time as the enactment of the Medicare ESRD entitlement in the US, new legislature in Australia provided coverage for all dialysis modalities and regimens – whether home or in-center – thus allowing home therapies to flourish in Australia while it plunged in the US5. By the early 2000s, the only countries with significant HHD usage among dialysis patients were Australia (11.1%), New Zealand (13.7%), and Turkey (11.1%)4.
Current Trends in HHD
Over the last ten years there has been a global resurgence in HHD owing to: (1) the introduction of novel HHD machines with simplified, patient-friendly technology, (2) growing clinical experience, (3) initiatives in patient empowerment and training, (4) emerging studies showing improved mortality and morbidity outcomes of more frequent HD, and (5) an appreciation for the enhanced quality of life of patients utilizing HHD.
According to the U.S. Renal Data System (USRDS) 2024 Annual Data Report (ADR), the percentage of prevalent patients performing home hemodialysis increased from 1.4% in 2010 to 2.38% in 2022 (Figure 3)3. In 2019, the US President signed an Executive Order launching the Advancing American Kidney Health Initiative, which has a goal of increasing the use of home dialysis by making it easier for patients to receive care at home. The initiative aims to have 80% of new American kidney failure patients in 2025 receiving dialysis in the home or receiving a transplant. From 2019 to 2020 alone, there was an 18.5% increase in the number of prevalent US patients performing HHD (relative to the 2.5% decrease in ICHD patients and 5.17% increase in PD patients)6.
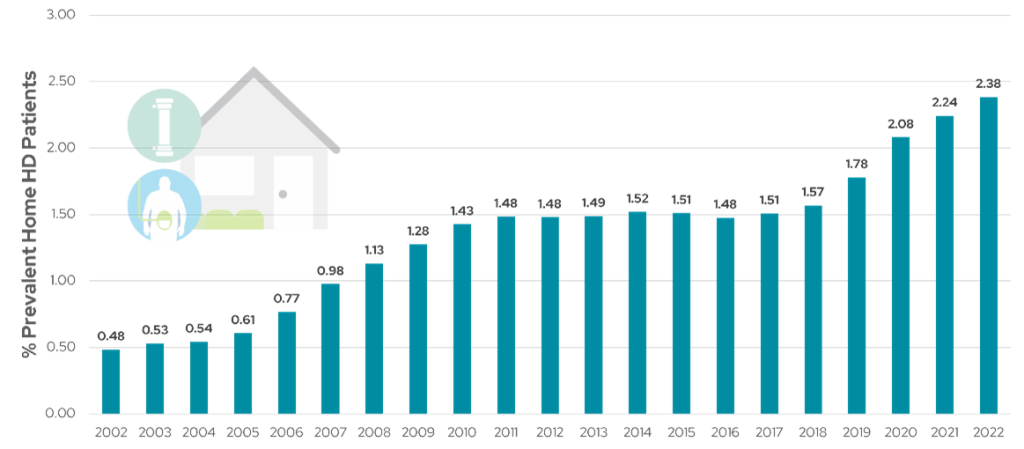
Figure 3: Percentage of prevalent US dialysis patients on home hemodialysis from 2002-2022 (Adapted from USRDS 2024 ADR3).
The use of HHD continues to be higher in many European and Pacific countries. As shown in Figure 4, 14.2% of patients in New Zealand and 7.7% of patients in Australia use HHD as of 20203. Finland, Netherlands, and Hong Kong also showed growth of HHD between 2011 and 2020.
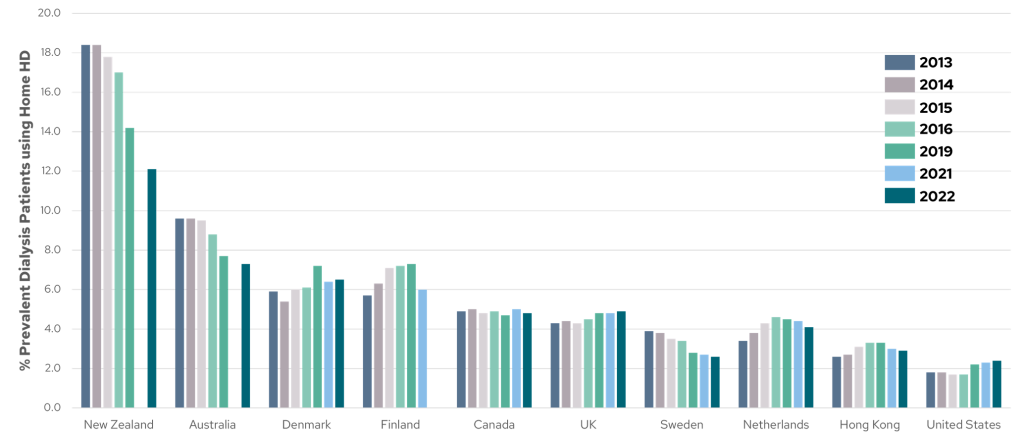
Figure 4: Percentage of prevalent dialysis patients on HHD in various countries around the world from 2013-2022 (Adapted from USRDS 2024 ADR3).
The renewed interest in home hemodialysis (HHD) and the emphasis on intensified HD warrants an in-depth analysis of the various modalities and prescriptions currently available and their impact on clinical outcomes and patient lifestyle. This module reviews intensified HD therapies, the relationship between dose, time, and frequency, and the clinical advantages and challenges of home HD.
References:
- Blagg CR. The early history of dialysis for chronic renal failure in the United States: a view from Seattle. Am J Kidney Dis. 2007;49(3):482-496. Available from: http://www.ncbi.nlm.nih.gov/pubmed/17336711.
- Bryan F. The National Dialysis Registry: Development of a Medical Registry of Patients on Chronic Dialysis, Final Report, June 1967-August 1976. Research Triangle Institute; 1976.
- United States Renal Data System. 2024 USRDS Annual Data Report: Epidemiology of Kidney Disease in the United States. National Institutes of Health, National Institute of Diabetes and Digestive and Kidney Diseases, Bethesda, MD, 2024.
- Kerr PG, Jaw J. Home Hemodialysis: What Is Old Is New Again. Contrib Nephrol. 2017;190:146-155.
- Agar JWM, Barraclough KA, Piccoli GB. Home haemodialysis: how it began, where it went wrong, and what it may yet be. J Nephrol. 2019;32(3):331-333.
- United States Renal Data System. 2022 USRDS Annual Data Report: Epidemiology of Kidney Disease in the United States. National Institutes of Health, National Institute of Diabetes and Digestive and Kidney Diseases, Bethesda, MD, 2022.
GMO-001412 Rev A 11/2024